Dr Ahsan Tariq , MBBS, MRCP (UK ) ongoing, IMT ( Internal Medicine Trainee, NHS England), GMC : 7805049
Dr Ahsan Tariq is a UK-registered medical doctor with a background in internal medicine and a focus on evidence-based research in cognitive health and nootropics. He critically reviews scientific studies, supplements, and ingredients to help readers make informed, safe, and effective choices for brain health and performance.
Introduction
Circulatory system health problems are the most common cause of death and disability worldwide, yet many people recognize them only after a crisis such as a heart attack or stroke. The circulatory system carries oxygen and nutrients through arteries, capillaries, and veins, returning blood to the heart and lungs. When any part of this network becomes narrowed, stiff, leaky, or inflamed, organs suffer silently for years before symptoms appear. According to the World Health Organization, cardiovascular diseases account for an estimated 17.9 million deaths each year, representing nearly one third of global mortality [1].
Data from the American Heart Association confirm that nearly half of adults in the United States have at least one major circulatory risk factor, often without awareness [2]. This blog post explains what circulatory system health problems are, how they develop, why they matter, and what science shows about prevention, treatment benefits, and risks. The aim is to move readers from simple awareness to practical action without oversimplifying the biology.
Understanding the topic
Circulatory system health problems include a spectrum of disorders that impair blood flow or pressure regulation. They can affect arteries that supply oxygen rich blood, veins that return deoxygenated blood, lymphatic channels, or the heart as a pump. Common arterial conditions are hypertension, atherosclerosis, coronary artery disease, cerebrovascular disease, and peripheral artery disease. Venous problems include chronic venous insufficiency and deep vein thrombosis. Structural defects such as aneurysms and inherited connective tissue disorders also fall within the category.
These conditions share underlying biology but differ in presentation. Atherosclerosis, for example, is now understood as a chronic inflammatory process in which low density lipoprotein particles accumulate in the arterial wall, trigger immune cells, and form plaque that can rupture [3]. Hypertension involves sustained pressure overload that strains the heart and small vessels, increasing the risk of twelve distinct cardiovascular events, from myocardial infarction to end stage renal disease, as demonstrated in a large cohort of 1.25 million patients [4]. Peripheral artery disease affects more than 200 million people globally and impairs limb blood flow, often silently because many patients mistake leg pain for aging [9]. Circulatory problems, therefore, are not one disease but a continuum of disorders that begin at the endothelium, the delicate cellular lining that releases nitric oxide to keep vessels flexible [17].
How it works
Healthy circulation depends on a balance between vascular tone, blood viscosity, and cardiac output. The endothelium coordinates dilation and constriction by releasing signaling molecules, most notably nitric oxide. When risk factors such as smoking, high glucose, or oxidized lipids damage endothelial cells, the vessels lose elasticity and become prone to spasm and plaque [18]. Chronic inflammation amplifies the injury; macrophages engulf oxidized cholesterol, become foam cells, and release cytokines that attract more immune cells, thickening plaques [27]. Over time plaque can calcify or rupture, exposing thrombogenic material that triggers clotting and sudden blockage.
Arterial dysfunction
In arteries the primary problem is often resistance and narrowing. High intraluminal pressure damages the elastic fibers of large arteries, leading to arterial stiffness and widened pulse pressure. Small resistance vessels remodel, perpetuating elevated blood pressure even when the heart is relaxed. Endothelial dysfunction reduces nitric oxide bioavailability and increases endothelin mediated constriction [19]. This state predicts future events independently of traditional risk factors.
Venous and microvascular dysfunction
Veins rely on valves and muscle pumps to return blood against gravity. Valve incompetence or obstruction creates pooling, inflammation, and skin changes typical of chronic venous disease. Microvascular dysfunction in capillaries precedes symptoms in diabetes and hypertension, limiting tissue perfusion despite open large arteries. The net effect is reduced oxygen delivery, ischemia, and eventual organ damage such as brain white matter lesions or kidney fibrosis.
Importance
Understanding circulatory system health problems matters because they dominate adult morbidity and strain health systems. In the most recent statistical update, cardiovascular disease remained the leading global killer, with ischemic heart disease and stroke still first and second causes of death in many countries [11]. Moreover, the lifetime risk for developing cardiovascular disease exceeds 50 percent for men and roughly one third for women in middle age, even when traditional risk is modest [25]. The social cost is also steep: lost productivity, dependence after stroke, and high expense for interventions such as bypass surgery, dialysis, and limb amputation.
Early identification also matters because damage begins decades before clinical events. Calcification scores on computed tomography can detect subclinical atherosclerosis years before angina [20]. Natriuretic peptide testing improves diagnosis of early heart failure when symptoms are nonspecific [16]. Without attention, silent plaque rupture can trigger myocardial infarction in people who felt healthy that morning.
Proven benefits
Preventive strategies consistently lower events, improve quality of life, and extend healthy years. Large meta analyses show that every 10 mmHg reduction in systolic pressure achieved with medication lowers risk of coronary events by about 20 percent and stroke by roughly 35 percent [6]. Lifestyle approaches provide complementary benefit. In the 2013 PREDIMED trial, a Mediterranean diet enriched with olive oil or nuts reduced combined cardiovascular events by about 30 percent compared with a low fat control [14]. Regular moderate activity improves endothelial function, lowers systemic inflammation, and reduces arterial stiffness [13].
Risk assessment tools help allocate benefit. Individuals with elevated coronary artery calcium scores receive larger absolute risk reduction from statins because their baseline risk is higher [20]. Comprehensive preventive care that includes smoking cessation, diet, exercise, and control of lipids and glucose reduces lifetime exposure to toxic risk factors, which is a dominant driver of disease [15]. Modern anti inflammatory therapy further reduces recurrent events, as seen in the CANTOS trial where interleukin 1 beta inhibition lowered cardiovascular events independent of lipids [21]. Even low dose colchicine, an inexpensive anti inflammatory, demonstrated lower rates of myocardial infarction and stroke in patients with chronic coronary disease [22].
Potential risks
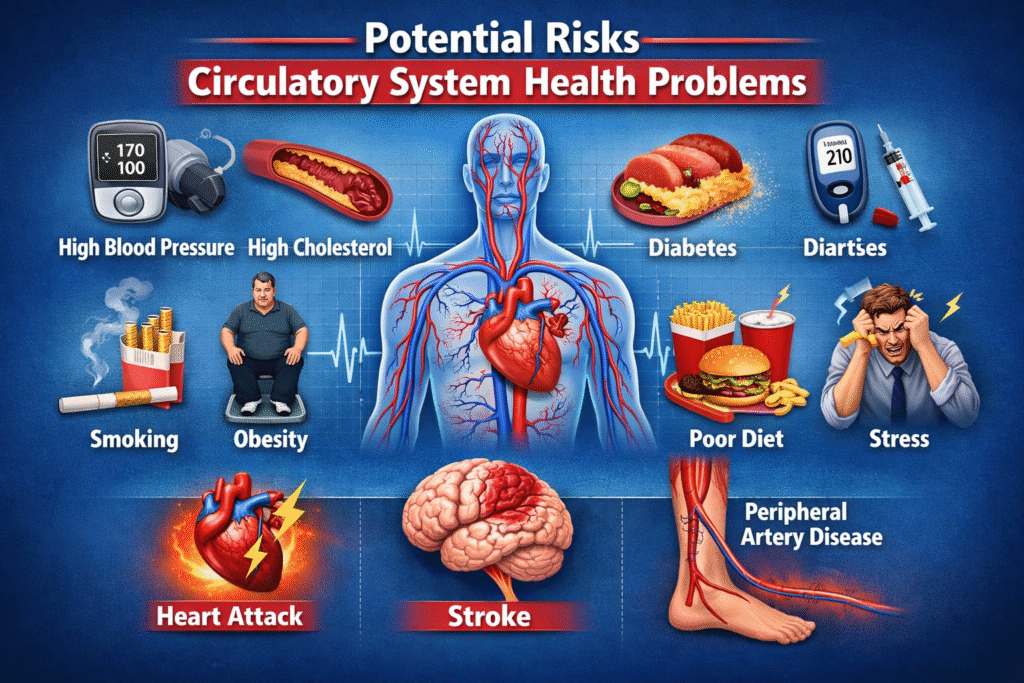
Circulatory system health problems progress silently but culminate in life threatening emergencies. Untreated hypertension damages the retina, kidneys, and cerebral vessels, leading to hemorrhagic stroke and dementia risk [4]. Unstable plaque can rupture, causing acute coronary occlusion within minutes. In peripheral artery disease, advanced limb ischemia can require amputation and shortens life expectancy comparable to aggressive cancers [8]. Stroke, by an updated definition, includes silent brain infarction that produces no obvious symptoms but predicts future major stroke and cognitive decline [10].
Treatments themselves carry potential harms when misapplied. Intensive blood pressure reduction may cause syncope or falls in frail elders [24]. Certain medications, such as beta blockers, may not reduce mortality after myocardial infarction in the modern reperfusion era and can precipitate fatigue or bradycardia [23]. Imaging tests, while valuable, involve radiation or contrast that require judicious use in low probability patients [30]. Ignoring venous thromboembolism risks results in pulmonary embolism, a common preventable hospital mortality.
Scientific evidence
Evidence spans population cohorts, mechanistic studies, and randomized trials. The INTERHEART case control study across 52 countries identified nine modifiable factors that explain more than 90 percent of heart attacks, including dyslipidemia, smoking, hypertension, diabetes, abdominal obesity, psychosocial stress, low fruit and vegetable intake, alcohol, and physical inactivity [15]. Inflammation is now considered causal, supported by trials targeting cytokines and proven reduction in events without lipid change [21]. Noninvasive imaging technologies such as coronary computed tomography angiography identify obstructive disease accurately and guide management decisions [30].
Large guidelines synthesize this evidence. The European Society of Cardiology recommends LDL cholesterol reduction based on total risk categories, with documented mortality benefits in secondary prevention [26]. United States professional societies emphasize a team based approach and advise coronary calcium scoring for borderline cases to refine decisions [7]. Experimental work on endothelial signaling earned the Nobel Prize and forms the mechanistic basis for modern vasodilator therapy [17].
Comparison of common circulatory system health problems
| Condition | Typical pathophysiology | Common early signs | Main long term risks | Key diagnostic test |
|---|---|---|---|---|
| Hypertension | Chronic pressure overload with arterial remodeling | Often none, occasional headache | Myocardial infarction, hemorrhagic stroke, renal failure [4] | Office and ambulatory cuff measurement [29] |
| Atherosclerosis | Lipid driven inflammatory plaque in arterial wall [27] | Exertional angina or none | Plaque rupture, unstable angina, sudden death | Coronary artery calcium scan or angiography [20] |
| Peripheral artery disease | Atherosclerotic stenosis of leg arteries | Intermittent claudication, atypical discomfort | Limb ischemia, amputation, cardiovascular death [8] | Ankle brachial index, duplex ultrasound |
| Venous insufficiency | Valve incompetence leading to pooling | Leg heaviness, edema, varicose veins | Skin ulcer, deep vein thrombosis | Duplex ultrasound, clinical severity score |
Benefits vs risks comparison
Interventions for Circulatory System Health Problems aim to restore flow, lower pressure, or prevent clotting. Each yields benefit but also adverse possibilities that must be weighed individually.
| Intervention domain | Main benefits | Observed risks or limitations | Evidence level |
|---|---|---|---|
| Blood pressure lowering | Reduced stroke, heart failure, renal decline; each 10 mmHg fall cuts mortality [6] | Hypotension, dizziness, renal hypoperfusion in older adults [24] | Strong randomized trials [5] |
| Intensive lipid control | Plaque stabilization, 20 to 25 percent relative risk reduction | Myalgia, rare rhabdomyolysis, drug interactions | ESC guidelines based on multiple trials [26] |
| Anti inflammatory therapy (colchicine) | Lower recurrent ischemic events in chronic coronary disease [22] | Gastrointestinal upset, rare agranulocytosis | Randomized CANTOS and LoDoCo2 trials [21] |
| Peripheral revascularization for PAD | Relief of claudication, limb salvage | Procedure failure, restenosis, contrast complications | Case series and controlled trials [8] |
The net balance favors therapy in medium and high risk patients, but precision is critical. Absolute benefit scales with baseline risk while absolute harm remains relatively constant, so people with modest risk may gain marginal benefit and experience more side effects.
Safe usage guidelines
Safe prevention follows stepwise assessment and monitoring. First, measure blood pressure correctly using a validated device and proper cuff size after five minutes rest; repeated out of office readings confirm hypertension [29]. Laboratory testing includes fasting lipids, glucose, creatinine, and high sensitivity C reactive protein in intermediate risk adults. Lifestyle forms the foundation: 150 minutes weekly of aerobic activity of moderate intensity, a plant forward diet low in sodium and refined carbohydrates, and abstinence from tobacco [7].
When medication is needed, begin with one agent at low dose, monitor electrolytes and renal function, and titrate slowly to <130/80 mmHg for most adults per contemporary guidelines [5]. Statins are dosed by intensity rather than target LDL alone, and patients should receive clear guidance about muscle symptoms and when to call a clinician [26]. Exercise should be supervised in people with known coronary disease, obstructive PAD, or recent procedures. Home exercise programs for claudication can improve pain free walking distance but must be graded to avoid injury [8].
For imaging, use risk based pathways. Coronary artery calcium scoring can reclassify intermediate risk patients and spare unnecessary medication, but routine whole body scans are discouraged because of incidental findings and radiation [20]. Noninvasive stress imaging is appropriate when symptoms or baseline abnormalities complicate ECG interpretation [30].
Who should avoid it
Not every intervention suits every patient. High intensity resistance training or sprint intervals should be avoided in people with severe aortic stenosis, uncontrolled arrhythmia, or known unstable plaque because sudden hemodynamic load can provoke ischemia [5]. Certain pharmacologic agents present sex specific concerns. Women with coronary artery disease often present atypically and may have nonobstructive plaque; aggressive antiplatelet regimens that benefit obstructive disease can increase bleeding without benefit [28].
Older adults with frailty and multiple medications are more susceptible to blood pressure medication induced falls, and the benefit of very low systolic targets diminishes in these groups [24]. Beta blocker therapy after myocardial infarction may lack benefit in patients without heart failure or arrhythmia, and should be reconsidered to avoid bradycardia and fatigue [23]. Patients with peptic ulcer disease should avoid nonsteroidal anti inflammatory drugs for pain relief because they raise bleeding risk in the setting of dual antiplatelet therapy.
Alternatives
When traditional pharmacology is contraindicated or insufficient, alternatives exist but require evidence based application. Stress reduction and adequate sleep improve autonomic balance and endothelial function, lowering blood pressure modestly across populations [12]. The Mediterranean diet stands out among dietary patterns for primary prevention, but other nutrient rich approaches like the DASH diet or whole food plant based plans also reduce pressure and lipids [14]. Supervised yoga and tai chi can improve heart rate variability and functional capacity in select patients.
Minimally invasive techniques such as supervised exercise therapy often postpone or replace peripheral revascularization in claudication [8]. For refractory angina, enhanced external counterpulsation and coronary sinus reducer devices offer symptom relief when revascularization is unsuitable. Dietary priorities that emphasize unsaturated fats, fiber, and minimal processed foods lower long term vascular risk independent of weight loss [12].
Expert opinions
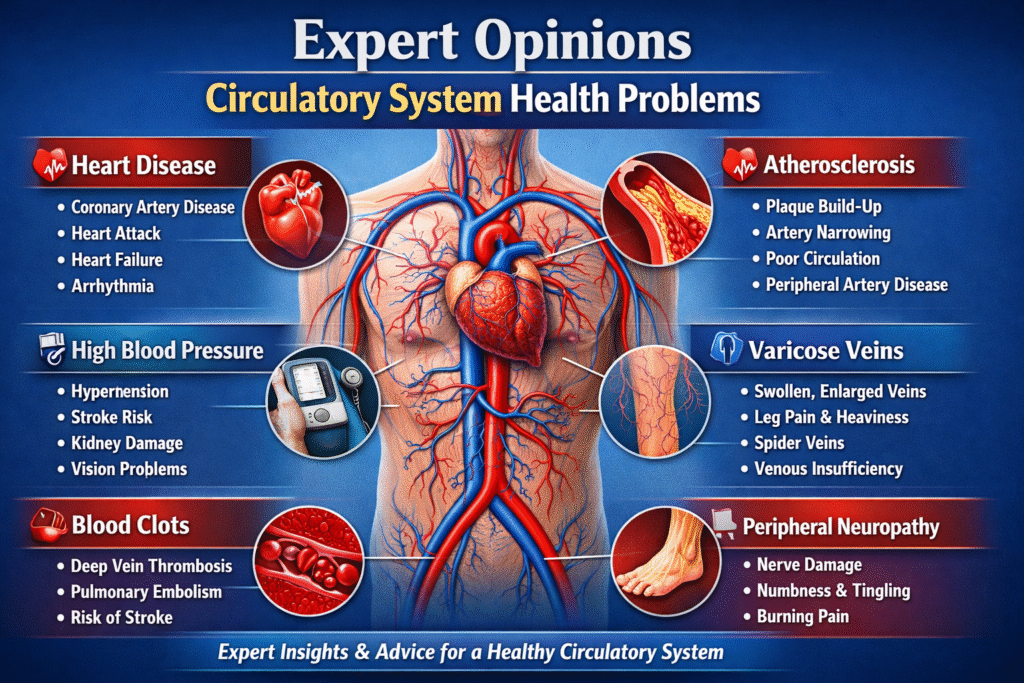
Professional societies converge on a message of early comprehensive risk management. The American College of Cardiology and American Heart Association state that prevention begins with assessing pooled cohort risk, then uses shared decision making to personalize diet, exercise, and pharmacotherapy [7]. European guidelines emphasize lifetime risk rather than ten year windows and recommend aggressive lipid lowering in very high risk patients, citing endothelial protection work that shows early lesions are reversible [13].
Vascular biology experts highlight that restoring endothelial health through nonpharmacologic means is central. They point to original discoveries that nitric oxide mediates vessel relaxation; preserving this pathway via diet, physical activity, and smoking cessation translates into measurable improvements in flow mediated dilation [17]. Imaging experts recommend coronary calcium screening in adults reluctant to start lifelong statins, enabling risk discussion rather than blanket prescribing [20]. Finally, outcomes researchers emphasize that public health policies targeting tobacco, sodium, and trans fats save more lives than individual interventions alone [15].
Key takeaways
Circulatory system health problems begin with endothelial injury and inflammation, progress silently, and drive most deaths worldwide [1]. Nine modifiable factors explain the majority of events, making prevention highly feasible [15]. Mediterranean diet, regular activity, and blood pressure and lipid control deliver substantial and durable benefits [14]. Treatment benefits outweigh risks when baseline risk is elevated, but intensity must be tailored to age, frailty, and comorbidities [24]. Noninvasive testing improves risk stratification but should be used selectively to avoid unnecessary harm [30]. Individual and policy level actions together reduce lifetime cardiovascular risk [12].
FAQs
What are the first warning signs of a circulatory system health problem?
Many people have no symptoms until a complication occurs. Early clues include intermittent leg pain when walking that resolves with rest, unexplained shortness of breath on exertion, swelling or heaviness in legs after standing, or frequent morning headaches. Silent hypertension is especially common; periodic cuff measurement is the only reliable way to detect it early [29].
Can young adults develop these problems?
Yes. Early plaque formation can begin in adolescence, especially with obesity, smoking, or family hyperlipidemia. Lifetime risk models show that even modest risk factors present before age 50 substantially raise future events [25]. Preventive habits adopted early preserve arterial compliance and reduce cumulative exposure.
Is all cholesterol treated the same?
No. Low density lipoprotein cholesterol drives atherosclerosis, while high density lipoprotein is less directly causal. Guidelines emphasize absolute risk and inflammation markers rather than cholesterol numbers alone [26]. Anti inflammatory therapies provide benefit independent of cholesterol lowering [21].
Are natural supplements enough to replace medication?
Dietary patterns and supplements such as plant sterols may modestly improve lipids, but they cannot replace medication in high risk people. Trials demonstrating event reduction used pharmacologic doses of statins, blood pressure agents, or targeted anti inflammatory drugs [6]. Lifestyle and medication are complementary rather than exclusive.
How often should blood pressure be checked?
Office checks at least annually are recommended after age 40. At home monitoring is valuable in diagnosed hypertension, using devices validated by international standards. More frequent monitoring is advised after starting therapy or during illness [5].
Conclusion
Circulatory system health problems represent a broad set of arterial and venous disorders rooted in endothelial dysfunction, inflammation, and pressure overload. Their global burden is immense, but evidence over decades shows that early detection and sustained management dramatically alter the trajectory. Benefits from diet, activity, and targeted medications are supported by rigorous trials; potential risks are real but manageable when therapy is personalized by age, frailty, and risk status.
Incorporating regular measurement, shared decision making, and guideline based interventions preserves heart, brain, and limb health across the lifespan. Protecting your circulatory health is therefore less about miracle cures and more about continuous, informed stewardship of the vessels that sustain every organ.
References
- World Health Organization. Cardiovascular diseases fact sheet. 2021.
- Benjamin EJ et al. Heart Disease and Stroke Statistics 2020 Update. Circulation. 2020
- Libby P. Inflammation in atherosclerosis. Nature. 2002
- Rapsomaniki E et al. Blood pressure and incidence of twelve cardiovascular diseases. Lancet. 2014
- Whelton PK et al. 2017 ACC AHA Hypertension Guideline. J Am Coll Cardiol. 2018
- Law MR et al. Blood pressure lowering drugs in prevention meta analysis. BMJ. 2009
- Arnett DK et al. 2019 ACC AHA Guideline on Primary Prevention of Cardiovascular Disease. Circulation. 2019
- Criqui MH et al. Peripheral artery disease epidemiology. Circ Res. 2015
- Fowkes FG et al. Global prevalence of peripheral artery disease. Lancet. 2013
- Sacco RL et al. Updated definition of stroke for the 21st century. Stroke. 2013
- Virani SS et al. Heart Disease and Stroke Statistics 2021 Update. Circulation. 2021
- Mozaffarian D et al. Dietary and policy priorities for cardiovascular health. Circulation. 2016
- Piepoli MF et al. 2016 European Guidelines on cardiovascular disease prevention. Eur Heart J. 2016
- Estruch R et al. Primary prevention with Mediterranean diet. N Engl J Med. 2013
- Yusuf S et al. Modifiable risk factors in myocardial infarction INTERHEART. Lancet. 2004
- Wang TJ et al. Natriuretic peptide testing in heart failure. Circulation. 2004
- Furchgott RF et al. Endothelial role in relaxation. Nature. 1980
- Higashi Y et al. Endothelial function and oxidative stress. Circ J. 2009
- Vanhoutte PM et al. Endothelial dysfunction and vascular disease. Acta Physiol. 2009
- Greenland P et al. Coronary artery calcium score for risk stratification. JAMA. 2004
- Ridker PM et al. Anti inflammatory therapy targeting IL 1 beta CANTOS. N Engl J Med. 2017
- Nidorf SM et al. Colchicine in chronic coronary disease. N Engl J Med. 2020
- Bangalore S et al. Beta blocker therapy after myocardial infarction. JAMA Intern Med. 2014
- Newman AB et al. Frailty and cardiovascular risk in PAD. Circulation. 2001
- Lloyd Jones DM et al. Lifetime risk of cardiovascular disease. JAMA. 2006
- Reiner Z et al. ESC EAS Guidelines for lipids. Eur Heart J. 2011
- Ross R. Atherosclerosis an inflammatory disease. N Engl J Med. 1999
- Shaw LJ et al. Sex differences in coronary artery disease. J Am Coll Cardiol. 2009
- Smulyan H et al. Blood pressure measurement techniques. JAMA. 1976
- Patel MR et al. Diagnostic performance of noninvasive imaging for CAD. N Engl J Med. 2015