Dr Ahsan Tariq , MBBS, MRCP (UK ) ongoing, IMT ( Internal Medicine Trainee, NHS England), GMC : 7805049
Dr Ahsan Tariq is a UK-registered medical doctor with a background in internal medicine and a focus on evidence-based research in cognitive health and nootropics. He critically reviews scientific studies, supplements, and ingredients to help readers make informed, safe, and effective choices for brain health and performance.
Introduction: What Is Joint Mobilization
Musculoskeletal disorders are among the most common causes of long-term pain and disability worldwide. According to global health data, conditions such as low back pain, neck pain, osteoarthritis, and joint injuries affect hundreds of millions of people annually [1]. These conditions frequently involve joint stiffness, limited movement, and functional restriction. When joints lose mobility, daily activities such as walking, lifting, bending, or even sitting for long periods can become uncomfortable or painful.
Manual therapy is widely recognized as a conservative and non-invasive treatment option for restoring movement and reducing pain [2]. Among these approaches, joint mobilization is one of the most researched and clinically applied techniques in physical therapy practice [3].
But what is joint mobilization exactly? Why do physical therapists use it so frequently? How does it work at a mechanical and neurological level? And what does the scientific evidence say about its safety and effectiveness?
This detailed, research-supported guide explains what is joint mobilization, how it works, why it matters, its proven benefits, potential risks, safety considerations, alternatives, and expert-backed recommendations.
Understanding What Is Joint Mobilization
To clearly understand what is joint mobilization, it is essential to understand how joints function in the human body.
A joint is a structure where two or more bones meet. Synovial joints such as the shoulder, knee, hip, ankle, and spine are designed for movement and flexibility. These joints rely on several components working together:
- Articular cartilage for smooth movement
- Synovial fluid for lubrication
- Joint capsule for stability
- Ligaments for structural support
- Surrounding muscles for active control
Normal joint movement requires both visible motion and subtle internal movements. Visible movement, such as bending your knee or raising your arm, is called osteokinematics. However, beneath this visible motion are smaller accessory movements known as arthrokinematics gliding, rolling, and spinning of joint surfaces [4].
When these accessory movements become restricted due to injury, inflammation, immobilization, or degenerative changes, the joint cannot move normally. Even if the muscles are strong, movement may feel stiff or painful.
Joint mobilization is a skilled manual therapy technique designed to restore these accessory movements using slow, controlled, passive forces applied by a trained professional [5].
Unlike manipulation, which involves a rapid thrust, joint mobilization uses graded, gentle movements within the joint’s natural range [6].
Historical Development Of Joint Mobilization
Modern joint mobilization techniques were largely shaped by pioneers such as Geoffrey Maitland and Freddy Kaltenborn, who developed structured approaches based on biomechanics and clinical reasoning [7].
Maitland introduced a grading system that categorizes mobilization intensity according to the patient’s pain response and tissue resistance [8]. This structured approach improved safety and reproducibility, making joint mobilization widely accepted in physical therapy education.
Over time, research expanded beyond biomechanics and began exploring neurological mechanisms of manual therapy [9]. Today, joint mobilization is supported by clinical guidelines for several musculoskeletal conditions [10].
The Maitland Grading System Explained In Depth
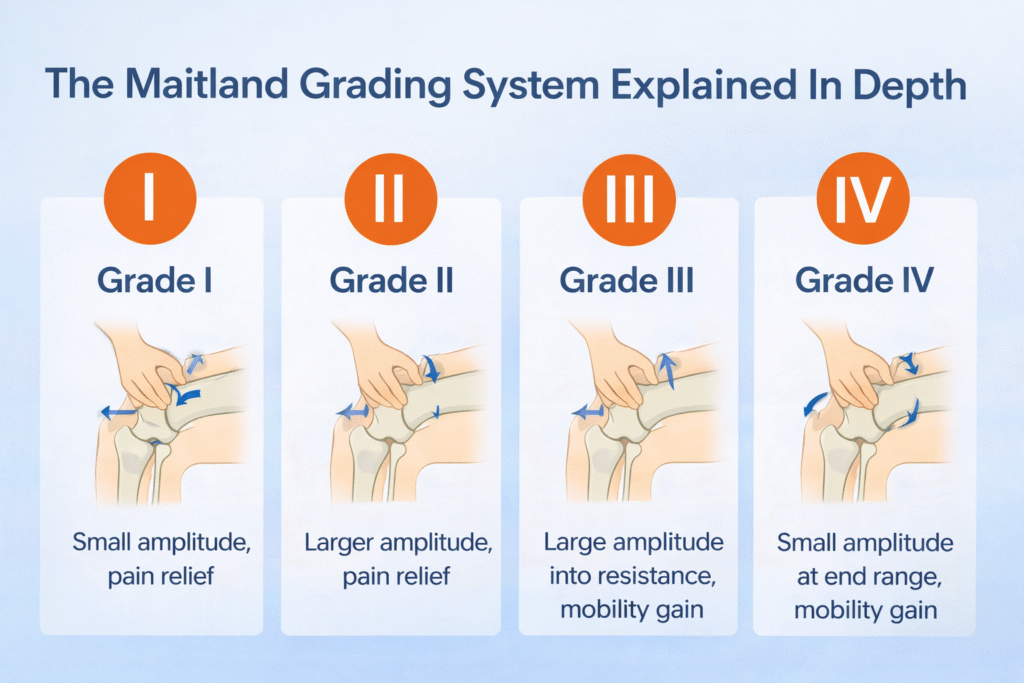
Joint mobilization is typically classified into four primary grades:
Grade I
This involves small amplitude oscillatory movement at the beginning of the available range. It is primarily used to reduce pain and calm irritated tissues. It does not stretch the joint capsule significantly but influences neurological pain pathways.
Grade II
This involves larger amplitude movement within the available range but not reaching tissue resistance. It is also primarily used for pain reduction and to improve joint lubrication.
Grade III
This involves large amplitude movement that reaches into tissue resistance. It is used to stretch capsular structures and improve joint mobility.
Grade IV
This involves small amplitude movement performed at the end range of motion. It is specifically designed to increase joint range by targeting capsular tightness.
Grades I and II primarily target pain modulation. Grades III and IV focus on improving mobility [8].
Biomechanics Of Joint Restriction
Joint stiffness can develop from several mechanisms:
- Capsular fibrosis following injury
- Scar tissue formation
- Synovial inflammation
- Prolonged immobilization
- Degenerative cartilage changes
When the joint capsule tightens, accessory glide is reduced. This creates abnormal joint loading patterns and increased stress on cartilage [11].
Joint mobilization mechanically stretches capsular tissues, improves elasticity, and restores normal arthrokinematic motion [12]. Improved glide reduces mechanical stress and allows muscles to function efficiently.
Neurophysiological Mechanisms Of Pain Relief
One of the most fascinating aspects of joint mobilization is how quickly pain can decrease.
Joint capsules contain mechanoreceptors that detect movement and pressure [13]. When mobilization stimulates these receptors, signals are sent to the spinal cord and brain. This activates descending inhibitory pathways that reduce pain perception [14].
Research shows that manual therapy can:
- Reduce central sensitization [15]
- Decrease muscle guarding [16]
- Improve motor unit recruitment [17]
- Influence cortical pain processing [18]
This means joint mobilization is not only mechanical it also alters how the nervous system processes pain.
Clinical Importance In Rehabilitation
Restricted joint mobility can disrupt the entire kinetic chain.
For example:
Limited ankle dorsiflexion can increase knee valgus stress and injury risk [19].
Hip stiffness can increase lumbar spine compression [20].
Thoracic spine restriction can impair shoulder elevation mechanics [21].
Clinical practice guidelines for neck pain and low back pain recommend manual therapy, including joint mobilization, as part of a comprehensive rehabilitation program [22][23].
Mobilization prepares the joint for strengthening exercises, improving long-term outcomes.
Proven Benefits Of Joint Mobilization
Pain Reduction
Systematic reviews demonstrate significant pain reduction in patients receiving joint mobilization for musculoskeletal conditions [24].
Improved Range Of Motion
Randomized trials show improvements in shoulder rotation, ankle dorsiflexion, and spinal mobility following mobilization [25].
Enhanced Functional Performance
Improved mobility translates into better walking, lifting, athletic movement, and daily task performance [26].
Osteoarthritis Management
Joint mobilization combined with exercise improves pain and function in knee osteoarthritis [27].
Post-Surgical Recovery
Mobilization reduces stiffness after joint replacement and ligament reconstruction surgeries [28].
Improved Proprioception
Mobilization enhances joint position sense and neuromuscular coordination [29].
Scientific Evidence Summary
A 2015 systematic review concluded that manual therapy combined with exercise produces superior outcomes compared to exercise alone in multiple musculoskeletal disorders [30].
Evidence supports joint mobilization in:
- Chronic low back pain
- Cervical dysfunction
- Shoulder impingement
- Knee osteoarthritis
- Ankle instability
While it is not a standalone cure, it significantly enhances rehabilitation when combined with exercise.
Benefits Vs Risks Comparison
| Benefits | Risks |
|---|---|
| Reduced pain [24] | Temporary soreness |
| Improved mobility [25] | Mild inflammation |
| Better joint mechanics | Rare symptom aggravation |
| Faster recovery [28] | Contraindicated in fractures |
| Improved proprioception [29] | Requires skilled application |
Most adverse effects are mild and temporary.
Potential Risks And Contraindications
Although generally safe, joint mobilization should be avoided in cases of:
- Acute fractures
- Active joint infection
- Malignancy in treatment area
- Severe osteoporosis
Relative caution is needed in hypermobility disorders and inflammatory arthritis flares [5].
Professional screening significantly reduces risk.
Joint Mobilization Vs Manipulation
Mobilization uses slow, controlled movement within physiological range. Manipulation involves high-velocity thrust beyond passive range and may produce cavitation sounds [6].
Mobilization is considered more conservative and generally lower risk.
Joint Mobilization Vs Stretching
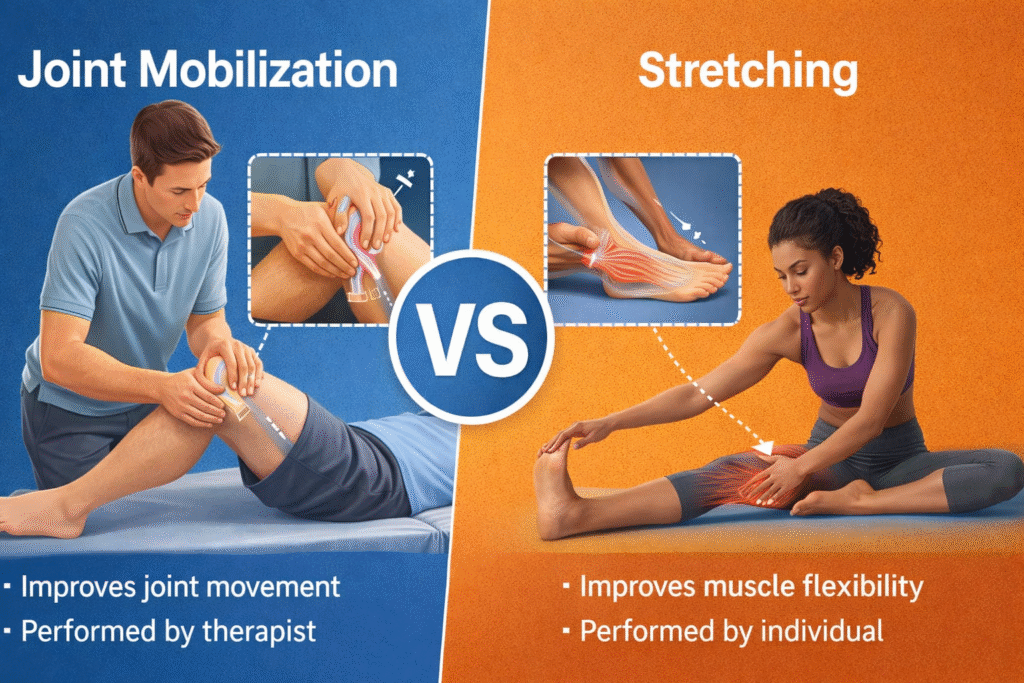
Stretching targets muscle tissue, improving flexibility. Joint mobilization specifically targets joint capsule and accessory movement [4].
Both are complementary in rehabilitation.
Who Should Avoid Joint Mobilization
Individuals with unstable fractures, severe bone density loss, or active infections should avoid mobilization. Medical evaluation is essential before treatment in complex conditions.
Long Detailed FAQs
What Is Joint Mobilization In Physical Therapy?
Joint mobilization is a graded, passive manual therapy technique used by physical therapists to restore joint mobility and reduce pain. It specifically targets accessory motion deficits that limit functional movement.
How Long Does It Take To See Improvement?
Some patients experience immediate pain reduction due to neurophysiological effects. However, long-term mobility gains typically require multiple sessions combined with strengthening exercises.
Is Joint Mobilization Safe For Older Adults?
Yes, when applied cautiously and modified for bone density and degenerative changes. It is commonly used in osteoarthritis management under professional supervision.
Key Takeaways
- What is joint mobilization? It is a controlled manual therapy technique used to restore joint mobility and reduce pain.
- It works through both biomechanical stretching and neurological pain modulation.
- It is supported by systematic reviews and clinical guidelines.
- It should be combined with strengthening and exercise.
- It is generally safe when performed by trained professionals.
Conclusion
Understanding what is joint mobilization allows patients and clinicians to make informed rehabilitation decisions. This evidence-based manual therapy approach restores accessory joint motion, reduces pain through neurological mechanisms, and improves functional performance.
When integrated into a structured rehabilitation program that includes strengthening, motor control training, and patient education, joint mobilization becomes a powerful tool for restoring movement and improving quality of life.
If you experience joint stiffness, restricted motion, or chronic musculoskeletal pain, consult a licensed healthcare professional to determine whether joint mobilization is appropriate for your condition.
References
- Global Burden of Disease Study 2019
- Vos T et al., Lancet, 2020
- American Physical Therapy Association Guidelines
- Neumann DA. Kinesiology of the Musculoskeletal System
- Maitland GD. Peripheral Manipulation
- Evans DW. Manual therapy definitions
- Kaltenborn FM. Manual Mobilization of the Joints
- Maitland grading system research
- Bialosky JE et al. Manual therapy mechanisms
- Neck Pain Clinical Practice Guidelines
- Joint capsule biomechanics studies
- Capsular stretching research
- Wyke B. Articular mechanoreceptors
- Descending pain modulation research
- Central sensitization studies
- Muscle reflex inhibition research
- Motor control improvement studies
- Neuroimaging manual therapy research
- Ankle dorsiflexion biomechanical study
- Hip-lumbar interaction research
- Thoracic mobility shoulder study
- Neck Pain Clinical Guidelines 2017
- Low Back Pain Clinical Guidelines 2021
- Systematic review manual therapy pain
- Shoulder and ankle RCT
- Functional mobility outcome trial
- Osteoarthritis manual therapy review
- Post-surgical rehabilitation study
- Proprioception and manual therapy research
- 2015 Manual Therapy Systematic Review

